The following article first appeared in The Pilot on April 12, 2019.
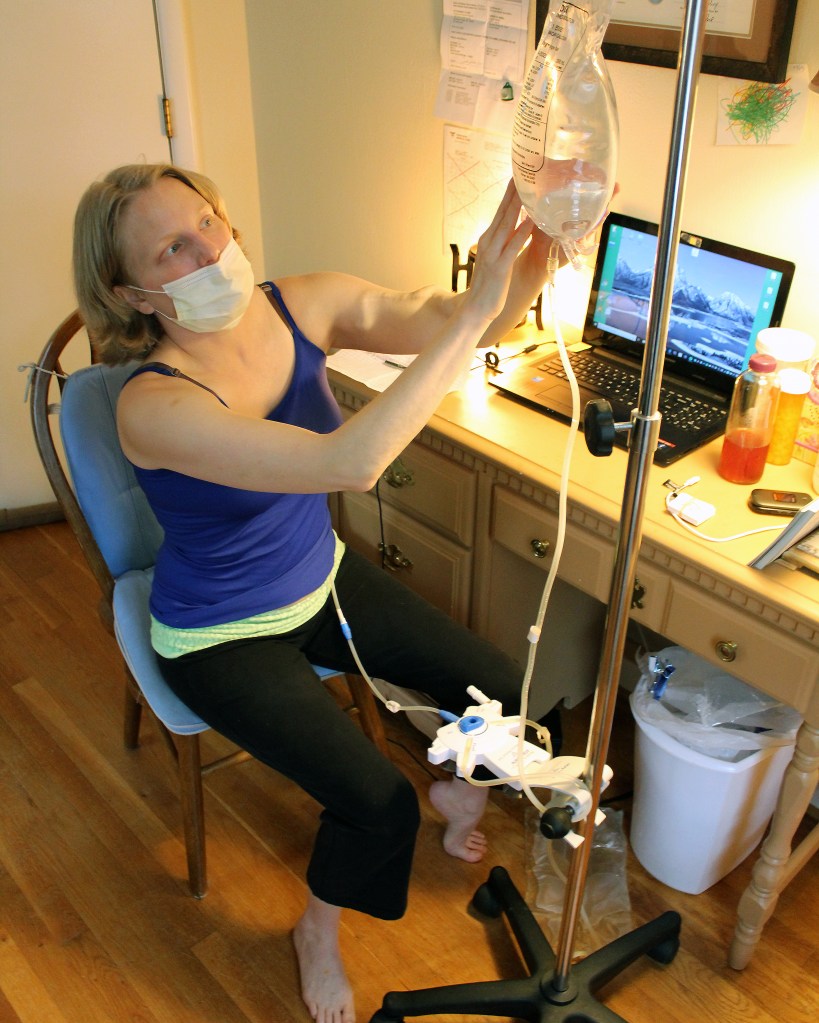
On Friday morning, Angela Gaskell used a needle to push nearly two pints of blood-cleansing fluid through a surgically implanted catheter in her stomach.
The treated blood traveled to her peritoneal membrane, which redirected the waste her kidneys can no longer filter out. After being ferried back by the fluid, the waste was drained from Gaskell’s body through the catheter. The whole process took about 10 minutes.
She repeated the ordeal four hours later, and repeated it again four hours after that. The routine will start over around the same time tomorrow and every day until Gaskell, 38, finds a replacement for her failing kidney.
The regimen has been part of Gaskell‘s daily life since she was diagnosed with end-stage renal disease in 2014. She believes her decision to immediately begin dialysis after her diagnosis is the reason she can still urinate.
“A lot of people on dialysis can’t pee,” she said. “I think because I started dialysis right away, that helped preserve some kidney function.”
For Gaskell, the manual approach, known as peritoneal dialysis, is preferable to hemodialysis, the more common form of treatment that requires several long visits to a clinic each week. Another option would require her to spend nine hours tethered to a whirring machine every evening at home.
Gaskell briefly tried the home device, sometimes called a night cycler, but she disliked how forcefully it sapped blood from her body. “It was painful,” she said.
The peritoneal method is not as convenient, but Gaskell said it allows her to be more independent.
“I don’t have to have this big machine in my room, and I don’t have to rely on electricity if there’s a storm,” said Gaskell, who currently lives with her mother near downtown Southern Pines.
Still, Gaskell said she must always “think 10 steps ahead” when planning her day. Her part-time job as a receptionist at Pinehurst Surgical Clinic is scheduled around her peritoneal exchanges. Long-distance travel is mostly off the table.
“I can’t go to the beach unless we’re staying at the beach,” she said.
Some trips are manageable with preparation. During a recent visit to the mountains, she drained the dialysate fluid from her body before leaving home and replenished it after reaching her destination.
Gaskell was once a professional ballerina. She performed with the Carolina Ballet, the Cincinnati Ballet and the Hungarian National Ballet.
In 2004, she was diagnosed with lupus. The autoimmune disease took a toll on Gaskell’s kidneys, derailing her promising future in ballet.
“My career was cut way short,” she said. “That was really hard because being a dancer was my identity.”

Gaskell is one of 27 Moore County residents on the national waitlist to receive a new kidney through the death of a registered donor. Several factors are used to determine a patient’s placement on the list, with small children taking precedence.
More than 3,160 people in North Carolina are on the list. Over 2,780 of them are in need of kidneys, making it the state’s most sought-after organ.
Data from the national Organ Procurement and Transplantation Network, which is overseen by the U.S. Department of Health and Human Services, shows that 193 kidney transplants have been performed so far this year at the state’s six transplant centers. All but 38 of the kidneys were harvested from non-living donors.
There are more than 5 million registered organ donors in the state, but the pool of usable body parts is significantly smaller than that. Kidneys can only be harvested from benefactors who are pronounced dead at a hospital. Organs cannot be taken from registered donors who die at home or in vehicle accidents.
Even when a donor dies on the operating table, there is no guarantee their kidneys will be fit for transplant. Nearly 450 of the state’s donated kidneys have been discarded by surgeons since 2014, the year Gaskell was placed on the waitlist.
Gaskell said it could be years before a cadaver that shares her O-negative blood type becomes available. On top of the wait, kidneys harvested from dead donors are less dependable than organs from living contributors.
“You’re better off with a living donor,” Gaskell said. “The chances of being healthier and having the kidney last longer are higher.”
An event will be held at the Shaw House in Southern Pines later this month to help match Gaskell with a living donor. She hopes the event, which is being called Spring for Angela, will also boost awareness for others in need of organ transplants.
Local donors and recipients of organs will speak about their experiences during the event. Gaskell thinks their success stories could persuade attendees to register to become organ donors.
According to the National Kidney Foundation, dialysis patients have an average life expectancy of five to 10 years. This year marks the fifth anniversary of the start of Gaskell’s treatment.
If she succeeds in her search for a living donor, Gaskell will still need to find a way to pay for the transplant. The procedure typically costs more than $414,000, only a portion of which is covered by insurance.
The National Foundation for Transplants is raising money to defray some of the potential costs associated with Gaskell’s surgery. Tax-deductible donations can be made through her profile on the foundation’s website.
